New Psoriasis treatments 2024
New Psoriasis Treatments 2024
Psoriasis is a chronic autoimmune condition characterized by the rapid buildup of skin cells, leading to scaling on the skin's surface. These scales often appear as red patches that can be itchy and sometimes painful. While the exact cause of psoriasis is not fully understood, it is believed to be related to an immune system issue with T cells and other white blood cells, called neutrophils, in the body. Psoriasis is not contagious and its severity can vary greatly from person to person. Common triggers for psoriasis flare-ups include infections, stress, cold weather, and certain medications.
When considering treatment options for psoriasis, it is important to consult with a healthcare provider to determine the most appropriate approach based on the severity and type of psoriasis, as well as the patient's overall health. Topical treatments, such as corticosteroids and vitamin D analogs, are commonly used for mild to moderate psoriasis. For more severe cases, phototherapy or systemic medications, including biologics, may be recommended. Recent advancements in medicine have led to the development of new biologic drugs that specifically target the immune system pathways involved in psoriasis, offering hope for better disease management. It is crucial for patients to discuss potential side effects and the long-term management plan with their healthcare provider before starting any new medication.

Treatment options
| Treatment option | Estimated cost | Efficacy | Eligibility |
|---|---|---|---|
| Topical treatments (corticosteroids, vitamin D analogues, etc.) | $10 - $100 | Mild to moderate efficacy | Mild to moderate psoriasis |
| Phototherapy (UVB light) | $100 - $500 | Moderate to high efficacy | Moderate to severe psoriasis |
| Methotrexate | $20 - $100 | Moderate to high efficacy | Moderate to severe psoriasis |
| Cyclosporine | $200 - $600 | Moderate to high efficacy | Severe psoriasis or rapid control needed |
| Acitretin | $300 - $800 | Moderate efficacy | Severe psoriasis or pustular psoriasis |
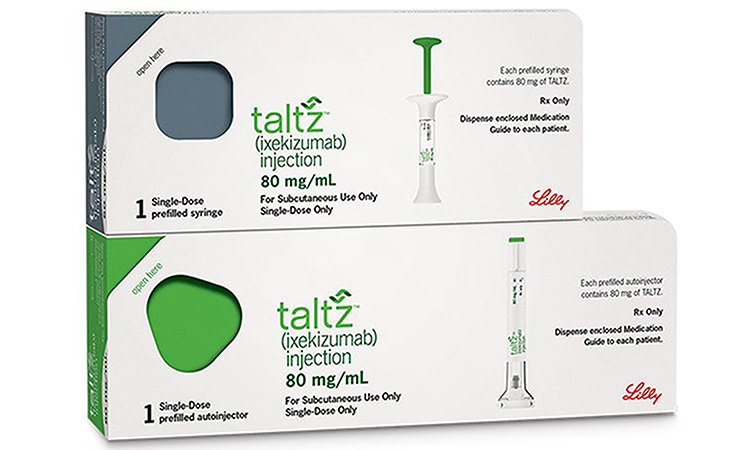
| Taltz (ixekizumab) | $4,000 - $5,000 | High efficacy | Moderate to severe plaque psoriasis |
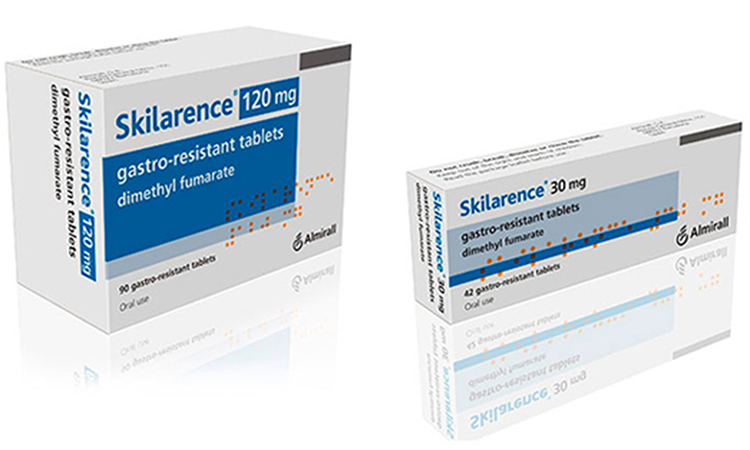
| Skilarence (dimethyl fumarate) | $1,000 - $1,500 | Moderate efficacy | Moderate to severe psoriasis |
| Tremfya (guselkumab) | $5,000 - $6,000 | High efficacy | Moderate to severe plaque psoriasis |
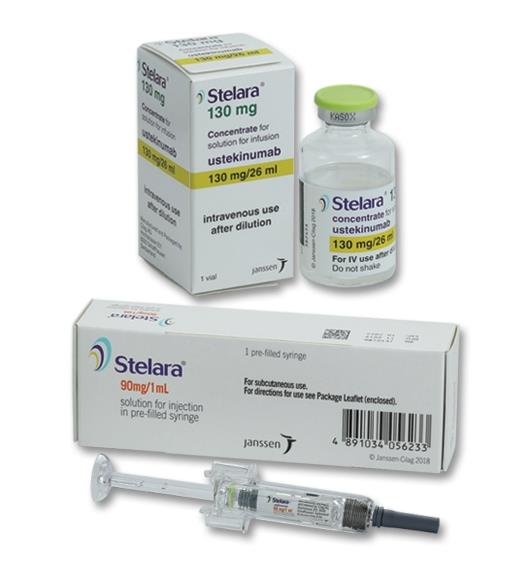
| Stelara (ustekinumab) | $9,000 - $11,000 | High efficacy | Moderate to severe plaque psoriasis |
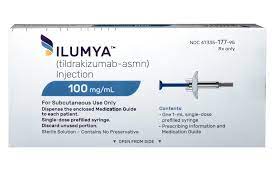
| Ilumya (tildrakizumab) | $2,000 - $3,000 | High efficacy | Moderate to severe plaque psoriasis |
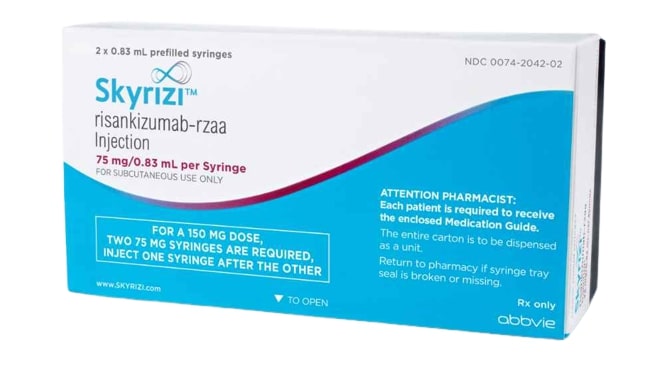
| Skyrizi (risankizumab) | $5,000 - $6,000 | High efficacy | Moderate to severe plaque psoriasis |
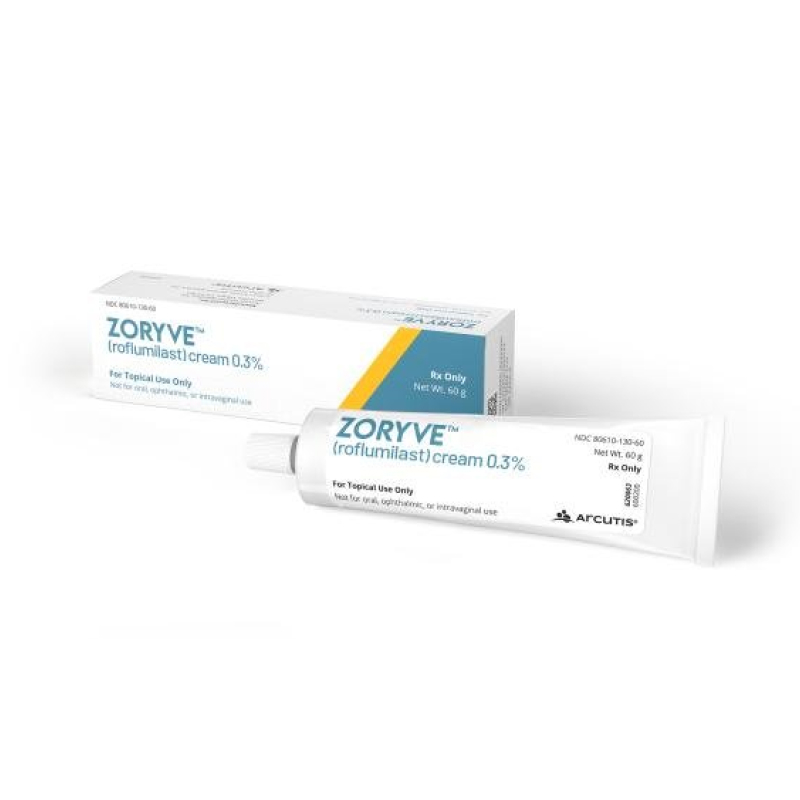
| Zoryve (roflumilast) | Not available | Experimental | Currently under investigation |
| Sotyktu (deucravacitinib) | $2,500 - $3,500 | High efficacy | Moderate to severe plaque psoriasis |
| Wezlana (biosimilar to Enbrel) | $1,000 - $1,500 | High efficacy | Moderate to severe plaque psoriasis |
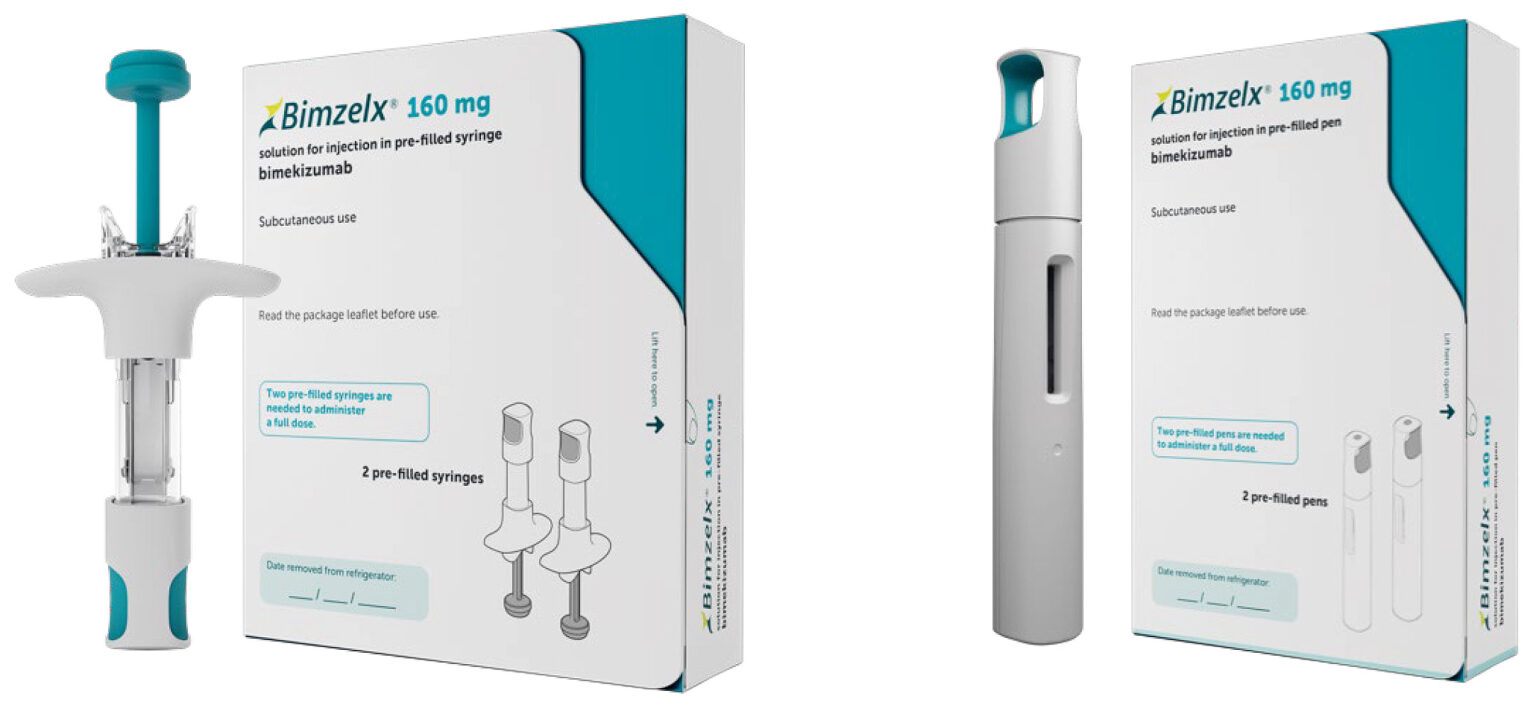
| Bimzelx (bimekizumab) | Not available | Experimental | Currently under investigation |
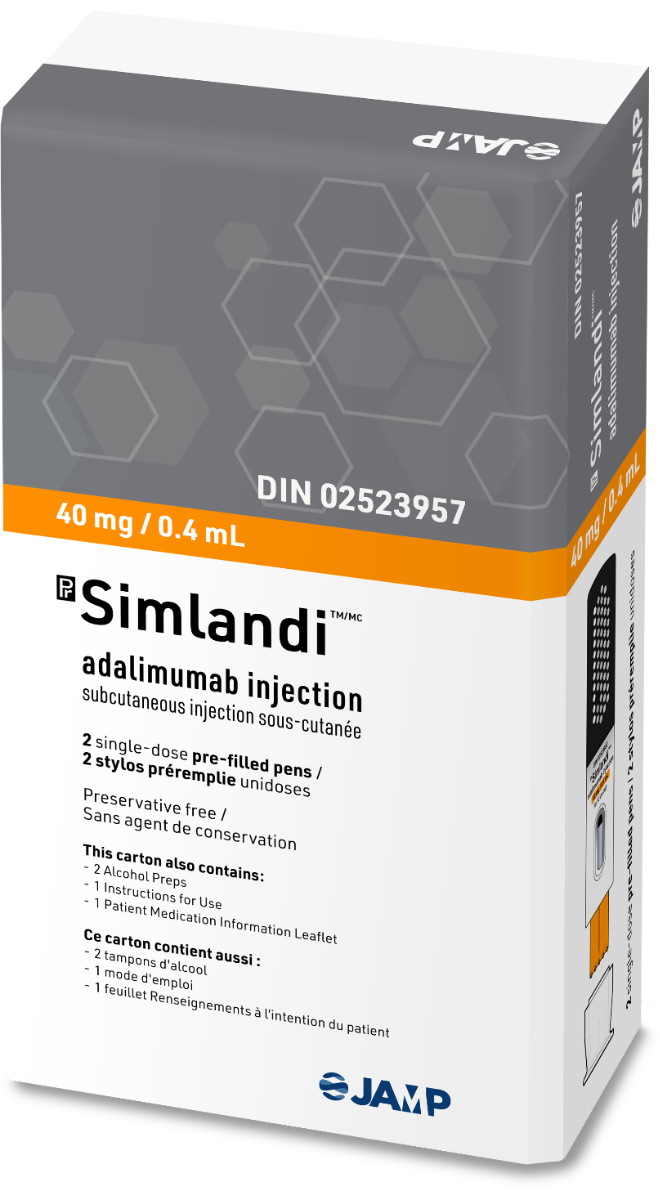
| Simlandi (biosimilar to Humira) | $1,000 - $1,500 | High efficacy | Moderate to severe plaque psoriasis |
Treatments options in detail
Topical Treatments
Topical treatments are often the first-line therapy for psoriasis, especially for mild to moderate cases. These include corticosteroids, which reduce inflammation and itching; vitamin D analogues such as calcipotriene, which help slow down skin cell growth; and topical retinoids like tazarotene, which may also help to control skin cell production. Additionally, coal tar and anthralin can be used to reduce scaling, though they are less commonly prescribed due to their potential to irritate the skin and stain clothing.
Phototherapy
Phototherapy or light therapy involves exposing the skin to ultraviolet light under medical supervision. This treatment can be administered as UVB phototherapy, including narrowband UVB therapy, which is the most common form, or psoralen plus ultraviolet A (PUVA) therapy, which combines the light-sensitizing medication psoralen with UVA light.
Systemic Medications
For moderate to severe cases of psoriasis or when topical treatments and phototherapy are ineffective, systemic medications that affect the entire body may be prescribed. These include methotrexate, cyclosporine, and acitretin. These medications can have significant side effects and often require regular blood tests to monitor for toxicity.
Biologic Agents
Biologic agents are a newer class of systemic drugs that target specific parts of the immune system that drive inflammation in psoriasis. These include tumor necrosis factor-alpha (TNF-alpha) inhibitors such as etanercept, adalimumab, and infliximab; interleukin 17 (IL-17) inhibitors such as secukinumab and ixekizumab (Taltz); interleukin 12 and 23 (IL-12/23) inhibitors such as ustekinumab (Stelara); and interleukin 23 (IL-23) inhibitors such as guselkumab (Tremfya), tildrakizumab (Ilumya), and risankizumab (Skyrizi).
Oral Small Molecules
Oral small molecules are a newer class of systemic treatments that can be taken by mouth. Apremilast (Otezla) is an example that reduces inflammation by inhibiting an enzyme known as phosphodiesterase 4 (PDE4). Deucravacitinib (Sotyktu) is another oral small molecule that selectively inhibits the tyrosine kinase 2 (TYK2) enzyme, which is involved in the inflammatory process of psoriasis.
Topical PDE4 Inhibitors
Roflumilast cream (Zoryve) is a topical PDE4 inhibitor approved for the treatment of plaque psoriasis, including in sensitive areas like the face and intertriginous areas. It offers a non-steroidal option for patients who may be concerned about the long-term use of topical steroids.
Interleukin Inhibitors
Several biologic agents target interleukins involved in the inflammatory process of psoriasis. These include bimekizumab (Bimzelx), which inhibits both IL-17A and IL-17F, and mirikizumab (Simlandi), which targets IL-23. These medications are administered via injection and are designed to reduce the signs and symptoms of psoriasis by modulating the immune response.
Off-Label and Investigational Treatments
Some medications may be used off-label for psoriasis, meaning they are not FDA-approved for this specific condition but have shown efficacy in some cases. These include certain immunosuppressants and other drugs that affect the immune system.
Experimental treatments for psoriasis are continually being researched. These may include new biologic agents, oral medications, or topical treatments that target different aspects of the immune system or skin cell production. Clinical trials are essential for determining the safety and efficacy of these potential new therapies.
Combination Therapy
Combination therapy, where two or more treatments are used together, can sometimes be more effective than using a single treatment alone. For example, using a topical corticosteroid with a vitamin D analogue may be more effective and reduce the side effects compared to using either treatment alone. Combining phototherapy with systemic treatments can also enhance the effectiveness of both therapies.
Lifestyle Modifications and Adjunctive Therapies
Lifestyle modifications, such as maintaining a healthy weight, avoiding smoking and excessive alcohol consumption, and managing stress, can also play a role in controlling psoriasis symptoms. Adjunctive therapies, including emollients for skin hydration, bath solutions, and dietary supplements, may provide additional symptomatic relief for some patients.
Dimethyl Fumarate (Skilarence)
Dimethyl fumarate (Skilarence) is an oral medication approved in some regions for the treatment of moderate to severe plaque psoriasis. It is thought to work by modulating the immune system, although its exact mechanism of action in psoriasis is not fully understood.
Janus Kinase (JAK) Inhibitors
Janus kinase (JAK) inhibitors are a class of medication that block the activity of one or more of the Janus kinase family of enzymes, interfering with the JAK-STAT signaling pathway, which is an important pathway in the inflammatory process of psoriasis. Tofacitinib is an example of a JAK inhibitor that is currently used off-label for psoriasis.
IL-23 Inhibitors
IL-23 inhibitors such as guselkumab (Tremfya), tildrakizumab (Ilumya), and risankizumab (Skyrizi) specifically target the IL-23 protein, which is involved in the pathogenesis of psoriasis. These drugs have been shown to be effective in reducing the severity of psoriasis symptoms and are administered by injection.
IL-17 Inhibitors
IL-17 inhibitors, such as secukinumab and ixekizumab (Taltz), block the action of interleukin-17, a cytokine that plays a key role in the inflammation associated with psoriasis. These medications have been effective in clinical trials and are also administered by injection.
IL-12/23 Inhibitors
Ustekinumab (Stelara) is an IL-12/23 inhibitor that targets two specific cytokines, IL-12 and IL-23, which are known to be involved in the inflammatory processes that contribute to psoriasis. Stelara has been shown to be effective in reducing the severity and extent of psoriatic lesions.
IL-17F Inhibitors
Bimekizumab (Bimzelx) is a novel biologic that inhibits both IL-17A and IL-17F, two cytokines involved in the inflammatory process of psoriasis. By targeting both cytokines, it has the potential to provide improved outcomes for patients with moderate to severe plaque psoriasis.
IL-23 p19 Inhibitors
Mirikizumab (Simlandi) is an investigational IL-23 p19 inhibitor that is being studied for the treatment of moderate to severe plaque psoriasis. It targets a subunit of the IL-23 cytokine, which is thought to play a crucial role in the chronic inflammation characteristic of psoriasis.
Anti-TNF Agents
Anti-TNF agents such as adalimumab, etanercept, and infliximab are biologics that block tumor necrosis factor-alpha (TNF-alpha), a cytokine that contributes to the inflammatory response in psoriasis. These medications have been widely used and are effective for many patients with moderate to severe psoriasis.
Emerging Therapies
New therapies are continually being developed and tested in clinical trials. These include novel biologics, JAK inhibitors, and other small molecules that may offer improved safety profiles, greater efficacy, or more convenient dosing options compared to existing treatments. It is important for patients to discuss the potential risks and benefits of emerging therapies with their healthcare provider.
Conclusion
The treatment of psoriasis is complex and individualized, often requiring a combination of therapies to achieve optimal control of symptoms. While many treatments are approved and widely used, ongoing research continues to expand the options available to patients, including those mentioned such as Taltz, Skilarence, Tremfya, Stelara, Ilumya, Skyrizi, Zoryve, Sotyktu, Wezlana, Bimzelx, and Simlandi. Patients should work closely with their healthcare providers to determine the best treatment plan for their specific condition.
Symptoms
Common Symptoms of Psoriasis
Psoriasis is primarily characterized by patches of abnormal skin. These patches are typically red, itchy, and scaly. The most common type of psoriasis, plaque psoriasis, features plaques of thickened, inflamed skin covered with silvery-white scales. These plaques may be painful and can crack and bleed. In severe cases, the skin at the joints may crack and bleed.
Another common symptom is the appearance of small scaling spots, particularly seen in children, known as guttate psoriasis. These spots are not as thick as the plaques seen in plaque psoriasis. Psoriasis can also manifest as discolored and pitted nails that may detach from the nail bed, a condition known as nail psoriasis.
Some individuals with psoriasis experience a burning or soreness around the affected areas. Itchiness is a frequent complaint, which can range from mild to severe and can lead to scratching, potentially exacerbating the condition. The psychological impact of psoriasis is also significant, with many individuals experiencing feelings of embarrassment or distress due to the visibility of their skin lesions.
Scalp Psoriasis
Scalp psoriasis is another common manifestation of the disease, where plaques of red, raised, scaly skin appear on the scalp. These can extend beyond the hairline onto the forehead, the back of the neck, and around the ears. Scalp psoriasis can be particularly uncomfortable due to tightness, soreness, and severe itching.
Psoriatic Arthritis
Some individuals with psoriasis may also develop psoriatic arthritis, which leads to joint pain, stiffness, and swelling. This can affect any joint in the body and can lead to permanent joint damage if not treated appropriately. The range of motion may also be affected in individuals with psoriatic arthritis.
Inverse Psoriasis
Inverse psoriasis is characterized by smooth patches of red, inflamed skin. It's more common in individuals who are overweight and is worsened by friction and sweating. Inverse psoriasis patches occur within skin folds, such as under the breasts, in the armpits, or around the groin, buttocks, and genitals.
Erythrodermic Psoriasis
Erythrodermic psoriasis is a particularly inflammatory form of psoriasis that often affects most of the body surface. It is a rare but severe type of psoriasis, causing widespread redness, severe itching, and pain. Individuals with this type of psoriasis may also experience an increase in heart rate and changes in body temperature. Because erythrodermic psoriasis can lead to severe illness, individuals experiencing symptoms should seek medical attention immediately.
Pustular Psoriasis
Pustular psoriasis is another rare form of the condition, characterized by white pustules surrounded by red skin. The pus within the blisters is non-infectious. Pustular psoriasis can be localized, often to the hands and feet (palmoplantar pustulosis), or generalized with widespread patches occurring randomly on any part of the body.
Additional Symptoms
Psoriasis symptoms can vary from person to person and can come and go in cycles, flaring for a few weeks or months, then subsiding for a time, or going into complete remission. Some individuals may also experience associated conditions, such as psoriatic arthritis, which can cause joint pain and stiffness.
It is also important to note that psoriasis can lead to or be associated with other health conditions, such as cardiovascular disease, diabetes, and depression. The inflammation associated with psoriasis can affect the entire body, and individuals with severe psoriasis may have an increased risk of heart attack and stroke.
Triggers and Aggravating Factors
Various triggers can initiate or exacerbate psoriasis symptoms, including infections, such as strep throat or skin infections, injury to the skin, such as a cut or scrape, bug bite, or severe sunburn, stress, which is one of the most common psoriasis triggers, cold weather, which can dry out the skin and lead to flare-ups, smoking, heavy alcohol consumption, and certain medications, including lithium, high blood pressure medications, and antimalarial drugs.
Understanding and recognizing the symptoms of psoriasis is crucial for timely diagnosis and management of the condition. If any of the above symptoms or triggers are present, it is advisable to consult with a healthcare provider for proper assessment and treatment options.
Cure
Understanding the Cure for Psoriasis
As of the current medical understanding, there is no definitive cure for psoriasis. Psoriasis is a chronic autoimmune condition that causes the rapid build-up of skin cells, leading to scaling on the skin's surface. The condition is characterized by cycles of remission and flare-ups over a patient's lifetime. While the exact cause of psoriasis is not fully understood, it is believed to be related to an immune system problem with T cells and other white blood cells, called neutrophils, in the body.
Treatment Goals for Psoriasis
The primary goals in managing psoriasis are to decrease inflammation and the rate of skin cell growth, to remove scales, and to smooth the skin. Treatments aim to reduce symptoms and improve the quality of life for those with the condition. A variety of treatment options exist that can help manage the symptoms and improve the appearance of the affected skin. These treatments include topical therapies, phototherapy, systemic medications, and biologic drugs.
Topical Treatments
Topical treatments are often the first line of defense against psoriasis and can be used alone in mild to moderate cases or in conjunction with other therapies for more severe cases. These include corticosteroids, vitamin D analogues, retinoids, calcineurin inhibitors, coal tar, anthralin, and moisturizers. Topical corticosteroids, in particular, are the most frequently prescribed medication for treating mild to moderate psoriasis. They reduce inflammation and relieve itching and may be used in combination with other treatments.
Phototherapy
Phototherapy or light therapy involves exposing the skin to ultraviolet light on a regular basis under medical supervision. This treatment can be administered in a health care provider's office, psoriasis clinic, or at home with a phototherapy unit. The key to success with light therapy is consistency. There are several types of phototherapy, including UVB phototherapy, narrowband UVB therapy, excimer laser, and PUVA (psoralen plus UVA).
Systemic Medications
For more severe cases of psoriasis or those that are resistant to other types of treatment, systemic medications are an option. These are prescription drugs that are taken orally or by injection and work throughout the body. They include methotrexate, cyclosporine, and acitretin. These medications can have serious side effects and are generally used for brief periods and may be alternated with other forms of treatment.
Biologics
Biologic drugs, or biologics, are a relatively new class of treatment for psoriasis and psoriatic arthritis. They are made from living cells cultured in a laboratory. Biologics target specific parts of the immune system that drive inflammation in psoriasis. These drugs are administered through injection or intravenous (IV) infusion. Examples include adalimumab (Humira), etanercept (Enbrel), infliximab (Remicade), and ustekinumab (Stelara). Due to their targeted nature, biologics may have fewer side effects than traditional systemic drugs, but they can be associated with an increased risk of infection.
Off-Label Medications and Treatments
Some medications used to treat other diseases have been found to be effective in treating psoriasis as well. These are known as off-label treatments and may include drugs used for the treatment of rheumatoid arthritis or inflammatory bowel disease. Off-label use of medications is a common and necessary practice in dermatology, especially when standard treatments are ineffective or unsuitable for the patient. However, it is important to note that off-label drug use should only be done under the guidance of a qualified healthcare provider.
Lifestyle Modifications and Complementary Therapies
Alongside medication, lifestyle modifications can play a significant role in managing psoriasis symptoms. These include maintaining a healthy weight, avoiding tobacco, managing stress, and following a nutritious diet. Some patients find relief with complementary therapies such as aloe vera, fish oil supplements, Oregon grape, and exposure to small amounts of sunlight. However, patients should consult with their healthcare provider before starting any complementary therapies to ensure they do not interfere with their primary treatments.
Research and Future Directions
Research into the treatment of psoriasis is ongoing, with new therapies and drugs being developed and tested. Advances in understanding the immune system's role in psoriasis have led to the development of new biologic drugs that are more effective and have fewer side effects. Additionally, research into gene therapy and other novel treatments offers hope for the future. However, until a definitive cure is found, the focus remains on controlling symptoms and improving the quality of life for those affected by psoriasis.
Conclusion
In summary, while there is no cure for psoriasis at present, there are many effective treatments available that can control the symptoms, prevent complications, and improve the quality of life for those with the condition. The choice of treatment depends on the severity of the condition, the size of the areas involved, the type of psoriasis, the patient's health and age, and the impact of the disease on the patient's quality of life. Patients should work closely with their healthcare provider to find the most suitable treatment plan.
Access Psoriasis medicines today
If Psoriasis medicines are not approved or available in your country (e.g. due to supply issues), you can access them via Everyone.org.
How Everyone.org works

Make an enquiry
Choose the medicine you want to access, answer a couple of questions, and upload your prescription to speed things up. We’ll get back to you within 24 hours.


Make an enquiry
Choose the medicine you want to access, answer a couple of questions, and upload your prescription to speed things up. We’ll get back to you within 24 hours.


Breeze through the paperwork
We'll guide you through the required documents for importing unapproved medicine, ensuring you have all the necessary information.


Get a personalized quote
We’ll prepare a quote for you, including medicine costs and any shipping, administrative, or import fees that may apply.


Receive your medicine
Accept the quote and we’ll handle the rest - sourcing and safely delivering your medicine.

Some text on this page has been automatically generated. Speak to your physician before you start a new treatment or medication.
Let's talk
If you have any questions, call us or send us a message through WhatsApp or email:
Contact us